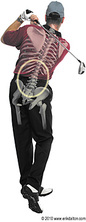
We watch it all the time on sports channels. How do they do it? That golf swing is actually a work of art. Requiring such a complex array of finely coordinated movements, it’s no wonder a golfer’s body is considered a ticking time bomb for acute injury or chronic pain.
Recent stats: 53 percent of male and 45 percent of female golfers suffer low back pain; 30 percent of professional golfers play injured; 33 percent of golfers are over the age of 50; and playing golf and another sport increases chance of injury by 40 percent.1
Recent stats: 53 percent of male and 45 percent of female golfers suffer low back pain; 30 percent of professional golfers play injured; 33 percent of golfers are over the age of 50; and playing golf and another sport increases chance of injury by 40 percent.1
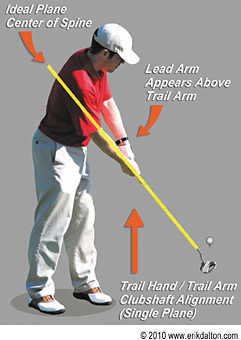
Researchers agree that a greater part of injuries affecting male golfers manifest in the low back and are related to improper swing mechanics and/or the repetitive nature of the game.2,3 The amateur or weekend golfer naturally experiences injuries due to improper swing mechanics, whereas the sports professional is more likely to fall victim to overuse injuries from obsessive repetitive movement patterns. When a high velocity rotary force couples with trunk sidebending (the crunch factor), the golfer’s spine and deep paravertebral tissues take a beating. No wonder low back pain (LBP) is the most frequent golfer complaint!
To hit the ball a great distance, the body must have the ability to rotate into and maintain a wide arc throughout the swing.
To hit the ball a great distance, the body must have the ability to rotate into and maintain a wide arc throughout the swing.
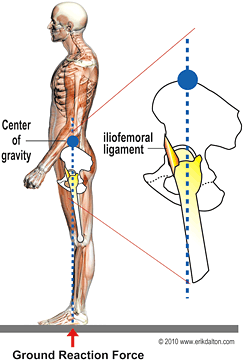
Manual therapy techniques that amplify range of hip turn allow a decrease in the amount of shoulder turn, thus reducing the amount of trunk flexion and sidebending during the downswing (the most damaging moment of the swing). If golfers lack full range of hip mobility due to an adhesive capsule, powerful torsional forces will travel up the kinetic chain through lumbopelvic ligaments, joint capsules and intervertebral discs. Motion-restricted facets and injured ligamentous tissue can neurologically inhibit deep spinal groove muscles such as rotatores, multifidus and intertransversarii leading to substitution patterns and low back instability.
Reported in the Journal of Science & Medicine in Sport (2008), University of South Australia researchers learned that golfers with LBP were overly dependent on erector spinae muscles for spinal stabilization rather than allowing load transfer to be distributed among more efficient lumbopelvic stabilizers such as quadratus lumborum, transverse abdominus, multifidus, hip extensors, and thoracolumbar fascia.4
Reported in the Journal of Science & Medicine in Sport (2008), University of South Australia researchers learned that golfers with LBP were overly dependent on erector spinae muscles for spinal stabilization rather than allowing load transfer to be distributed among more efficient lumbopelvic stabilizers such as quadratus lumborum, transverse abdominus, multifidus, hip extensors, and thoracolumbar fascia.4
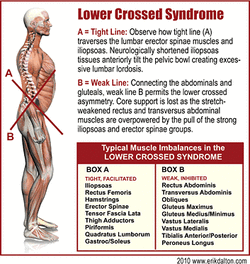
They theorized that the brain, sensing weakness, is forced to recruit global muscles (lumbar erectors and obliques) to offset for the weakened deep spinal stabilizers. The question is, “What mechanism causes the deep lumbopelvic stabilizers to weaken?”
Reconnecting the Disconnect
The body’s myofascial system is built from a continuous arrangement of tissues designed to function in organized patterns, not as isolated muscle groups. When operating properly, energy is competently transmitted via force-coupling through a reaction chain rooted in the ground. Motor unit recruitment only becomes isolated to a precise muscle group when the brain senses a system disconnect and calls in “the subs.” For example, during a golf swing, if a fibrosed hip capsule were blocking energy transfer up the kinetic chain, normal force-coupling would suffer due to lack of mobility of the femoral head in the acetabulum.
Reconnecting the Disconnect
The body’s myofascial system is built from a continuous arrangement of tissues designed to function in organized patterns, not as isolated muscle groups. When operating properly, energy is competently transmitted via force-coupling through a reaction chain rooted in the ground. Motor unit recruitment only becomes isolated to a precise muscle group when the brain senses a system disconnect and calls in “the subs.” For example, during a golf swing, if a fibrosed hip capsule were blocking energy transfer up the kinetic chain, normal force-coupling would suffer due to lack of mobility of the femoral head in the acetabulum.
(Fig 3) The therapist must first mobilize the fixated joint in all three cardinal planes, and then move up the kinetic chain to assess and correct any sacroiliac or lumbar compensation that may be driving the golfer’s back pain.
Successful treatment of golf-related injuries not only necessitates golf swing modifications and functional rehab, but, in most cases, restoration of proper lumbar lordosis. Too much or too little curve results in unwarranted torsional and compressive loads through the thoracolumbar and lumbosacral junctions. The myoskeletal approach starts by correcting lower crossed muscle imbalance patterns followed by restoration of “joint-play” to fixated low back, sacroiliac and thoracic articulations.
Read More ~
http://erikdalton.com/media/published-articles/toolbox-of-touch-the-mambo-of-golfing/
Successful treatment of golf-related injuries not only necessitates golf swing modifications and functional rehab, but, in most cases, restoration of proper lumbar lordosis. Too much or too little curve results in unwarranted torsional and compressive loads through the thoracolumbar and lumbosacral junctions. The myoskeletal approach starts by correcting lower crossed muscle imbalance patterns followed by restoration of “joint-play” to fixated low back, sacroiliac and thoracic articulations.
Read More ~
http://erikdalton.com/media/published-articles/toolbox-of-touch-the-mambo-of-golfing/
 RSS Feed
RSS Feed